结核与肺部疾病杂志 ›› 2022, Vol. 3 ›› Issue (4): 309-314.doi: 10.19983/j.issn.2096-8493.20220011
收稿日期:2022-01-28
出版日期:2022-08-20
发布日期:2022-08-16
通信作者:
吕良敬
E-mail:lu_liangjing@163.com
基金资助:
Li Yuan, Guo Ruru, Lyu Liangjing( )
)
Received:2022-01-28
Online:2022-08-20
Published:2022-08-16
Contact:
Lyu Liangjing
E-mail:lu_liangjing@163.com
Supported by:摘要:
结缔组织病是引起多系统功能障碍的自身免疫病,结核病是危害人民生命健康的重要传染病。结缔组织病患者患结核病风险较一般人群高,其临床表现不典型,诊疗难度大,且预后差。作者针对结缔组织病合并结核病的流行状况、危险因素、临床特点、筛查与治疗策略进行综述,为结缔组织病合并结核病的筛查、预防和控制提供最新的研究进展。
中图分类号:
郦源, 郭茹茹, 吕良敬. 结缔组织病合并结核病的研究进展[J]. 结核与肺部疾病杂志, 2022, 3(4): 309-314. doi: 10.19983/j.issn.2096-8493.20220011
Li Yuan, Guo Ruru, Lyu Liangjing. Research progress of connective tissue disease and tuberculosis comorbidity[J]. Journal of Tuberculosis and Lung Disease, 2022, 3(4): 309-314. doi: 10.19983/j.issn.2096-8493.20220011
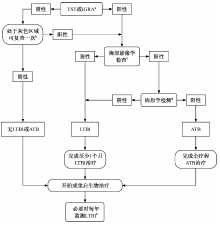
图1
CTD患者结核病筛查流程 注 TST:结核菌素皮肤试验; IGRA:γ-干扰素释放试验; LTBI:结核分枝杆菌潜伏感染; ATB:活动性结核病; a:满足以下任一条件的CTD患者必须采用IGRA检测:(1)有卡介苗接种史;(2)来自非结核分枝杆菌病高流行地区;(3)长期使用GC或ISA; b:灰色区域指TST在5~10mm或QFT的IFN-γ 在0.045~0.35IU/ml; c:对于TST或IGRA筛查阴性,但有结核临床指征患者,也可考虑胸部X线检查; d:获取呼吸道(例如,痰液、支气管肺泡灌洗液)或其他临床上适合于抗酸杆菌涂片和分枝杆菌培养的样本,必要时可采用Xpert等分子诊断技术; e:在结核低风险地区,出现新的结核病暴露时重新筛查LTBI,结核中高风险地区,每年筛查1次
| [1] | World Health Organization.Global tuberculosis report 2021Geneva:World Health Organization, 2021. |
| [2] |
Getahun H, Matteelli A, Chaisson RE, et al. Latent Mycobacterium tuberculosis infection. N Engl J Med, 2015, 372(22): 2127-2135. doi: 10.1056/NEJMra1405427.
doi: 10.1056/NEJMra1405427 URL |
| [3] |
王馨仪. 系统性红斑狼疮患者结核感染相关因素分析. 南昌: 南昌大学, 2020. doi: 10.27232/d.cnki.gnchu.2020.000331.
doi: 10.27232/d.cnki.gnchu.2020.000331 |
| [4] |
吴杰炜. 结缔组织疾病并发结核发病率及相关危险因素的meta分析. 重庆: 重庆医科大学, 2019. doi: 10.19613/j.cnki.1671-3141.2019.28.023.
doi: 10.19613/j.cnki.1671-3141.2019.28.023 |
| [5] |
Anton C, Machado FD, Ramirez JMA, et al. Latent tuberculosis infection in patients with rheumatic diseases. J Bras Pneumol, 2019, 45(2): e20190023. doi: 10.1590/1806-3713/e20190023.
doi: 10.1590/1806-3713/e20190023 |
| [6] |
Liu X, Zhang L, Zhang F, et al. Prevalence and Risk Factors of Active Tuberculosis in Patients with Rheumatic Diseases: A Multi-center, Cross-Sectional Study in China. Emerg Microbes Infect, 2021: 1-36. doi: 10.1080/22221751.2021.2004864.
doi: 10.1080/22221751.2021.2004864 |
| [7] |
Pettipher C, Benitha R. Tuberculosis in biologic users for rheumatic diseases: results from the South African Biologics Registry (SABIO). Ann Rheum Dis, 2020, 79(2): 292-299. doi: 10.1136/annrheumdis-2019-216128.
doi: 10.1136/annrheumdis-2019-216128 pmid: 31791950 |
| [8] |
Balbi GGM, Machado-Ribeiro F, Marques CDL, et al. The interplay between tuberculosis and systemic lupus erythematosus. Curr Opin Rheumatol, 2018, 30(4): 395-402. doi: 10.1097/bor.0000000000000493.
doi: 10.1097/bor.0000000000000493 URL |
| [9] |
Clayton K, Polak ME, Woelk CH, et al. Gene Expression Signatures in Tuberculosis Have Greater Overlap with Autoimmune Diseases Than with Infectious Diseases. Am J Respir Crit Care Med, 2017, 196(5): 655-656. doi: 10.1164/rccm.201706-1248LE.
doi: 10.1164/rccm.201706-1248LE URL |
| [10] |
González-Naranjo LA, Coral-Enríquez JA, Restrepo-Escobar M, et al. Factors associated with active tuberculosis in Colombian patients with systemic lupus erythematosus: a case-control study. Clin Rheumatol, 2021, 40(1): 181-191. doi: 10.1007/s10067-020-05225-x.
doi: 10.1007/s10067-020-05225-x URL |
| [11] |
Long W, Cai F, Wang X, et al. High risk of activation of latent tuberculosis infection in rheumatic disease patients. Infect Dis (Lond), 2020, 52(2): 80-86. doi: 10.1080/23744235.2019.1682187.
doi: 10.1080/23744235.2019.1682187 |
| [12] |
Sundbaum JK, Arkema EV, Bruchfeld J, et al. Tuberculosis in Biologic-naïve Patients With Rheumatoid Arthritis: Risk Factors and Tuberculosis Characteristics. J Rheumatol, 2021, 48(8): 1243-1250. doi: 10.3899/jrheum.201251.
doi: 10.3899/jrheum.201251 URL |
| [13] |
Aibana O, Huang CC, Aboud S, et al. Vitamin D status and risk of incident tuberculosis disease: A nested case-control study, systematic review, and individual-participant data meta-analysis. PLoS Med, 2019, 16(9): e1002907. doi: 10.1371/journal.pmed.1002907.
doi: 10.1371/journal.pmed.1002907 |
| [14] |
Xiao X, Da G, Xie X, et al. Tuberculosis in patients with systemic lupus erythematosus-a 37-year longitudinal survey-based study. J Intern Med, 2021, 290(1): 101-115. doi: 10.1111/joim.13218.
doi: 10.1111/joim.13218 pmid: 33259665 |
| [15] |
Cantini F, Niccoli L, Capone A, et al. Risk of tuberculosis reactivation associated with traditional disease modifying anti-rheumatic drugs and non-anti-tumor necrosis factor biologics in patients with rheumatic disorders and suggestion for clinical practice. Expert Opin Drug Saf, 2019, 18(5): 415-425. doi: 10.1080/14740338.2019.1612872.
doi: 10.1080/14740338.2019.1612872 URL |
| [16] |
Lim CH, Chen HH, Chen YH, et al. The risk of tuberculosis disease in rheumatoid arthritis patients on biologics and targeted therapy: A 15-year real world experience in Taiwan. PLoS One, 2017, 12(6): e0178035. doi: 10.1371/journal.pone.0178035.
doi: 10.1371/journal.pone.0178035 |
| [17] |
Cheng CF, Huang YM, Lu CH, et al. Prednisolone dose during treatment of tuberculosis might be a risk factor for mortality in patients with systemic lupus erythematosus: a hospital-based cohort study. Lupus, 2019, 28(14): 1699-1704. doi: 10.1177/0961203319882759.
doi: 10.1177/0961203319882759 pmid: 31640531 |
| [18] |
Brode SK, Jamieson FB, Ng R, et al. Increased risk of mycobacterial infections associated with anti-rheumatic medications. Thorax, 2015, 70(7): 677-682. doi: 10.1136/thoraxjnl-2014-206470.
doi: 10.1136/thoraxjnl-2014-206470 URL |
| [19] |
Cantini F, Blandizzi C, Niccoli L, et al. Systematic review on tuberculosis risk in patients with rheumatoid arthritis receiving inhibitors of Janus Kinases. Expert Opin Drug Saf, 2020, 19(7): 861-872. doi: 10.1080/14740338.2020.1774550.
doi: 10.1080/14740338.2020.1774550 URL |
| [20] |
Wang X, Wong SH, Wang XS, et al. Risk of tuberculosis in patients with immune-mediated diseases on biological therapies: a population-based study in a tuberculosis endemic region. Rheumatology (Oxford), 2019, 58(5): 803-810. doi: 10.1093/rheumatology/key364.
doi: 10.1093/rheumatology/key364 URL |
| [21] |
Ai JW, Zhang S, Ruan QL, et al. The Risk of Tuberculosis in Patients with Rheumatoid Arthritis Treated with Tumor Necrosis Factor-α Antagonist: A Metaanalysis of Both Randomized Controlled Trials and Registry/Cohort Studies. J Rheumatol, 2015, 42(12): 2229-2237. doi: 10.3899/jrheum.150057.
doi: 10.3899/jrheum.150057 URL |
| [22] |
Sartori NS, Picon P, Papke A, et al. A population-based study of tuberculosis incidence among rheumatic disease patients under anti-TNF treatment. PLoS One, 2019, 14(12): e0224963. doi: 10.1371/journal.pone.0224963.
doi: 10.1371/journal.pone.0224963 |
| [23] |
Cantini F, Nannini C, Niccoli L, et al. Risk of Tuberculosis Reactivation in Patients with Rheumatoid Arthritis, Ankylosing Spondylitis, and Psoriatic Arthritis Receiving Non-Anti-TNF-Targeted Biologics. Mediators Inflamm, 2017, 2017: 8909834. doi: 10.1155/2017/8909834.
doi: 10.1155/2017/8909834 |
| [24] |
Wallace DJ, Ginzler EM, Merrill JT, et al. Safety and Efficacy of Belimumab Plus Standard Therapy for Up to Thirteen Years in Patients With Systemic Lupus Erythematosus. Arthritis Rheumatol, 2019, 71(7): 1125-1134. doi: 10.1002/art.40861.
doi: 10.1002/art.40861 |
| [25] |
Lopez Velazquez M, Highland KB. Pulmonary manifestations of systemic lupus erythematosus and Sjögren’s syndrome. Curr Opin Rheumatol, 2018, 30(5): 449-464. doi: 10.1097/bor.0000000000000531.
doi: 10.1097/BOR.0000000000000531 pmid: 29985183 |
| [26] |
Mira-Avendano I, Abril A, Burger CD, et al. Interstitial Lung Disease and Other Pulmonary Manifestations in Connective Tissue Diseases. Mayo Clin Proc, 2019, 94(2): 309-325. doi: 10.1016/j.mayocp.2018.09.002.
doi: S0025-6196(18)30704-3 pmid: 30558827 |
| [27] |
Zayat AS, Mahmoud K, Md Yusof MY, et al. Defining inflammatory musculoskeletal manifestations in systemic lupus erythematosus. Rheumatology (Oxford), 2019, 58(2): 304-312. doi: 10.1093/rheumatology/key277.
doi: 10.1093/rheumatology/key277 URL |
| [28] |
Lin W, Chen P. Tubercular meningitis in patients with systemic lupus erythematosus: clinical characteristics, risk factors, and outcomes of 10 patients. Clin Rheumatol, 2020, 39(4): 1141-1145. doi: 10.1007/s10067-020-04940-9.
doi: 10.1007/s10067-020-04940-9 URL |
| [29] |
Wong SH, Gao Q, Tsoi KK, et al. Effect of immunosuppressive therapy on interferon γ release assay for latent tuberculosis screening in patients with autoimmune diseases: a systematic review and meta-analysis. Thorax, 2016, 71(1): 64-72. doi: 10.1136/thoraxjnl-2015-207811.
doi: 10.1136/thoraxjnl-2015-207811 URL |
| [30] |
Soare A, Gheorghiu AM, Aramă V, et al. Risk of active tuberculosis in patients with inflammatory arthritis receiving TNF inhibitors: a look beyond the baseline tuberculosis screening protocol. Clin Rheumatol, 2018, 37(9): 2391-2397. doi: 10.1007/s10067-017-3916-y.
doi: 10.1007/s10067-017-3916-y URL |
| [31] |
Kim HW, Kwon OC, Han SH, et al. Positive conversion of interferon-γ release assay in patients with rheumatic diseases treated with biologics. Rheumatol Int, 2020, 40(3): 471-479. doi: 10.1007/s00296-019-04510-6.
doi: 10.1007/s00296-019-04510-6 URL |
| [32] |
Pyo J, Cho SK, Kim D, et al. Systemic review: agreement between the latent tuberculosis screening tests among patients with rheumatic diseases. Korean J Intern Med, 2018, 33(6): 1241-1251. doi: 10.3904/kjim.2016.222.
doi: 10.3904/kjim.2016.222 URL |
| [33] |
Jeong DH, Kang J, Jung YJ, et al. Comparison of latent tuberculosis infection screening strategies before tumor necrosis factor inhibitor treatment in inflammatory arthritis: IGRA-alone versus combination of TST and IGRA. PLoS One, 2018, 13(7): e0198756. doi: 10.1371/journal.pone.0198756.
doi: 10.1371/journal.pone.0198756 |
| [34] |
Holroyd CR, Seth R, Bukhari M, et al. The British Society for Rheumatology biologic DMARD safety guidelines in inflammatory arthritis-Executive summary. Rheumatology (Oxford), 2019, 58(2): 220-226. doi: 10.1093/rheumatology/key207.
doi: 10.1093/rheumatology/key207 URL |
| [35] |
Aabye MG, Latorre I, Diaz J, et al. Dried plasma spots in the diagnosis of tuberculosis: IP-10 release assay on filter paper. Eur Respir J, 2013, 42(2): 495-503. doi: 10.1183/09031936.00129412.
doi: 10.1183/09031936.00129412 URL |
| [36] |
Villar-Hernández R, Latorre I, Mínguez S, et al. Use of IFN-γ and IP-10 detection in the diagnosis of latent tuberculosis infection in patients with inflammatory rheumatic diseases. J Infect, 2017, 75(4): 315-325. doi: 10.1016/j.jinf.2017.07.004.
doi: S0163-4453(17)30248-7 pmid: 28751171 |
| [37] |
Clifford V, Tebruegge M, Zufferey C, et al. Serum IP-10 in the diagnosis of latent and active tuberculosis. J Infect, 2015, 71(6): 696-698. doi: 10.1016/j.jinf.2015.08.001.
doi: 10.1016/j.jinf.2015.08.001 pmid: 26271898 |
| [38] |
Zhao Y, Yang X, Zhang X, et al. IP-10 and RANTES as biomarkers for pulmonary tuberculosis diagnosis and monitoring. Tuberculosis (Edinb), 2018, 111: 45-53. doi: 10.1016/j.tube.2018.05.004.
doi: 10.1016/j.tube.2018.05.004 URL |
| [39] |
Cho SK, Kim D, Won S, et al. Safety of resuming biologic DMARDs in patients who develop tuberculosis after anti-TNF treatment. Semin Arthritis Rheum, 2017, 47(1): 102-107. doi: 10.1016/j.semarthrit.2017.01.004.
doi: 10.1016/j.semarthrit.2017.01.004 URL |
| [40] |
Hejazi ME, Ahmadzadeh A, Khabbazi A, et al. Tuberculin skin test conversion in patients under treatment with anti-tumor necrotizing factor alpha agents. BMC Infect Dis, 2020, 20(1): 464. doi: 10.1186/s12879-020-05166-5.
doi: 10.1186/s12879-020-05166-5 URL |
| [41] |
Garziera G, Morsch ALB, Otesbelgue F, et al. Latent tuberculosis infection and tuberculosis in patients with rheumatic diseases treated with anti-tumor necrosis factor agents. Clin Rheumatol, 2017, 36(8): 1891-1896. doi: 10.1007/s10067-017-3714-6.
doi: 10.1007/s10067-017-3714-6 pmid: 28589321 |
| [42] |
Sterling TR, Njie G, Zenner D, et al.Guidelines for the Treatment of Latent Tuberculosis Infection: Recommendations from the National Tuberculosis Controllers Association and CDC, 2020 MMWR Recomm Rep, 2020, 69(1): 1-11. doi: 10.15585/mmwr.rr6901a1.
doi: 10.15585/mmwr.rr6901a1 pmid: 32053584 |
| [43] |
Lee J, Kim E, Jang EJ, et al. Efficacy of Treatment for Latent Tuberculosis in Patients Undergoing Treatment with a Tumor Necrosis Factor Antagonist. Ann Am Thorac Soc, 2017, 14(5):690-697. doi: 10.1513/AnnalsATS.201608-647OC.
doi: 10.1513/AnnalsATS.201608-647OC URL |
| [44] |
Chen YM, Liao TL, Chen HH, et al. Three months of once-weekly isoniazid plus RFPapentine (3HP) in treating latent tuberculosis infection is feasible in patients with rheumatoid arthritis. Ann Rheum Dis, 2018, 77(11): 1688-1689. doi: 10.1136/annrheumdis-2018-213097.
doi: 10.1136/annrheumdis-2018-213097 URL |
| [45] |
Nam SH, Oh JS, Hong S, et al. Early discontinuation of tofacitinib in patients with rheumatoid arthritis co-treated with RFPampin for latent tuberculosis. Joint Bone Spine, 2020, 87(5): 475-479. doi: 10.1016/j.jbspin.2020.04.010.
doi: 10.1016/j.jbspin.2020.04.010 URL |
| [46] |
Kim YJ, Kim YG, Shim TS, et al. Safety of resuming tumour necrosis factor inhibitors in patients who developed tuberculosis as a complication of previous TNF inhibitors. Rheumatology (Oxford), 2014, 53(8): 1477-1481. doi: 10.1093/rheumato-logy/keu041.
doi: 10.1093/rheumato-logy/keu041 URL |
| [47] |
Cantini F, Prignano F, Goletti D.Restarting biologics and management of patients with flares of inflammatory rheumatic disorders or psoriasis during active tuberculosis treatment J Rheumatol Suppl, 2014, 91:78-82. doi: 10.3899/jrheum.140106.
doi: 10.3899/jrheum.140106 URL |
| [48] |
Prabu V, Agrawal S. Systemic lupus erythematosus and tuberculosis: a review of complex interactions of complicated diseases. J Postgrad Med, 2010, 56(3): 244-250. doi: 10.4103/0022-3859.68653.
doi: 10.4103/0022-3859.68653 pmid: 20739781 |
| [1] | 卢水华. 关注结核病共患病已成为公共卫生的需要[J]. 结核与肺部疾病杂志, 2022, 3(4): 255-260. |
| [2] | 古力米娜·阿布力米提, 麦维兰江·阿不力米提, 地尔木拉提·吐逊, 刘振江, 何懿, 苏伟, 欧喜超. 2021年喀什地区肺结核患者利福平耐药影响因素分析[J]. 结核与肺部疾病杂志, 2022, 3(4): 269-273. |
| [3] | 杨震, 雷囡, 赵飞, 何艳萍, 林娜, 张治国. 北京市昌平区高等院校新生结核分枝杆菌潜伏感染状况调查及潜伏感染者预防性治疗效果分析[J]. 结核与肺部疾病杂志, 2022, 3(4): 274-280. |
| [4] | 董昭良, 姚黎明, 李领娣, 王连波, 姚晓伟, 李卓, 刘丰胜, 贾晨光. 保守方法治疗轻型脊柱结核的临床疗效[J]. 结核与肺部疾病杂志, 2022, 3(4): 281-286. |
| [5] | 李义帅, 秦学博, 李香兰, 魏兰, 段小亮, 张磊, 陈亮, 李建行. 电视辅助胸腔镜手术与开胸手术治疗难治性空洞性肺结核的效果分析[J]. 结核与肺部疾病杂志, 2022, 3(4): 292-295. |
| [6] | 李军霞, 孟艺哲, 张亚楠, 陈颜强, 赵青. 12例结核性神经根脊髓炎的临床特征及磁共振成像特点分析[J]. 结核与肺部疾病杂志, 2022, 3(4): 296-299. |
| [7] | 胡娟, 周燕, 杨澄清. 支气管结核患者焦虑、抑郁心理状况与行电子支气管镜治疗依从性的相关性分析[J]. 结核与肺部疾病杂志, 2022, 3(4): 305-308. |
| [8] | 钱晓文, 翟晓文. 造血干细胞移植与结核病[J]. 结核与肺部疾病杂志, 2022, 3(4): 315-319. |
| [9] | 张晓林, 李锋. 肺结核致呼吸衰竭研究进展[J]. 结核与肺部疾病杂志, 2022, 3(4): 320-324. |
| [10] | 刘玉坤, 郭智. 慢性髓系白血病与结核病共病研究进展[J]. 结核与肺部疾病杂志, 2022, 3(4): 325-327. |
| [11] | 何燕超, 揭志军. 综合医院活动性肺结核的早期筛查策略[J]. 结核与肺部疾病杂志, 2022, 3(4): 334-337. |
| [12] | 周伊南, 朱惠莉. 慢性阻塞性肺疾病合并肺结核的研究进展[J]. 结核与肺部疾病杂志, 2022, 3(4): 338-342. |
| [13] | 陈木兴, 范欣欣, 陈晓红, 林友飞, 黄明翔, 陈力舟, 吴迪. T淋巴细胞亚群检测在新型冠状病毒肺炎临床应用价值中的研究进展[J]. 结核与肺部疾病杂志, 2022, 3(4): 343-346. |
| [14] | 龚道敏, 朱凌, 田甜, 钟浈. 肺癌合并肺结核患者预感性悲伤影响因素分析[J]. 结核与肺部疾病杂志, 2022, 3(3): 193-197. |
| [15] | 徐翠玲, 蒋钰辉, 徐芳. 超前镇痛护理干预对肺结核胸部术后镇痛的效果分析[J]. 结核与肺部疾病杂志, 2022, 3(3): 198-202. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||
 京公安网备11010202008787号
ip访问总数: ip当日访问总数: 当前在线人数:
京公安网备11010202008787号
ip访问总数: ip当日访问总数: 当前在线人数:
 本作品遵循Creative Commons Attribution 3.0 License授权许可
本作品遵循Creative Commons Attribution 3.0 License授权许可